What the medical community calls desynchronosis has always plagued us who cheat gravity for a living. I think it first became a serious topic for flight safety studies following the China Airlines 006 crew who almost lost a perfectly good Boeing 747 over the Pacific. It can also be used as an excuse. The NASA study quoted below cites Korean Air 801 as a case where fatigue was causal, and yet it really wasn't. Whatever you call it, you need to understand it, recognize it, and know how to combat it.
— James Albright
Updated:
2014-03-28
Desynchronosis, by the way, is simply the desynchronization of one's body clock with the rest of the world. It has two forms: jet lag and shift lag. Jet lag you know. Shift lag is what shift workers going from day to night shift work, or night to day shift work, experience.
I think I've actually fallen asleep twice in the pilot's seat in my almost 35 years flying. The first time was in a T-37 trying to build time, the need for sleep had nothing to do with jet lag. The second time was in an Air Force Gulfstream III. I woke after flying halfway around the world up to a Russian air defense controller yelling at me, see Flying Where the Bullets Aren't. I consider myself a pretty conscientious pilot and don't tolerate anything not flight related in my cockpits. And yet there I was. Jet lag?
1 — Sleep and circadian rhythms
2 — Desynchronosis and jet lag

1
Sleep and circadian rhythms
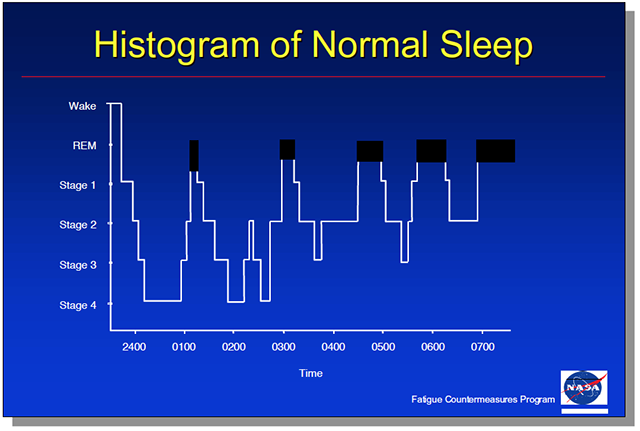
- It is widely believed that sleep is a time when the brain and the body shut off and then re-engage upon awakening. Actually, sleep is a highly complex physiological process during which the brain and body alternate between periods of extreme activity and quiet, but are never “shut off.” Sleep is composed of two distinct states: NREM, or non-rapid eye movement, and REM, or rapid eye movement, sleep. These two sleep states are as different from each other as they are from wakefulness.
- During NREM sleep, physiological and mental activities slow (e.g., heart rate and breathing rate slow and become regular). NREM sleep is divided into four stages, with the deepest sleep occurring during stages 3 and 4. There is usually very little mental activity during NREM stages 3 and 4. If awakened during this deep sleep, an individual may take sometime to wake up and then continue to feel groggy, sleepy, and perhaps disoriented for 10–15 minutes. This phenomenon is called sleep inertia.
- REM sleep is associated with an extremely active brain that is dreaming, and with bursts of rapid eye movements (probably following the activity of the dream); during REM sleep, the major motor muscles of the body are paralyzed. If awakened during REM sleep, individuals can often provide detailed reports of their dreams.
- Over the course of a typical night, NREM and REM sleep occur in a cycle, with about 60 minutes of NREM sleep followed by about 30 minutes of REM sleep. This 90-minute cycle repeats itself throughout a typical sleep period. However, most deep sleep (i.e., NREM stages 3 and 4) occurs in the first third of the night, and REM periods are shorter early in the night and then become longer and occur more regularly later in the sleep period. Overall, about 25% of sleep time is spent in REM sleep and about 50% is spent in NREM stage 2.
Source: NASA, pg. 10
You spend about a quarter of your sleep in the Rapid Eye Movement (REM) phase where your major motor muscles are paralyzed and you have those vivid dreams. But this isn't your deep sleep, that happens during another quarter of your sleep time known as Non-REM stages 3 and 4. You normally have 60 or so minutes of Non-REM stages 1 and 2, stages 3 and 4, back to stages 1 and 2, and then 30 minutes of REM sleep.
Circadian Rhythms
The mechanism that mediates the interdependence of human physiology with environmental cycles of light and dark has been referred to as the circadian timing system (CTS). It is generally accepted that the CTS synchronizes physiological and behavioral rhythms to a circadian period (circa, about; dies, a day) and that the phase of these rhythms can be reset by the influence of the environmental light/dark cycle.
Source: USAARL, pg. 323
Light/Dark Cycle
- The human body uses predictable environmental events such as sunrise and sunset to maintain a consistent internal organization of physiological functions. Peak levels of physiological rhythms are specifically timed to occur at the appropriate phase of the daily light/dark (LD) cycle.
- This internal synchronization of physiological rhythmicity results in the availability of metabolic energy, neurotransmitter synthesis, enzyme activity, and hormone production at critical times of the day.
Source: USAARL, pg. 323
Physiological and Behavioral Rhythms Exhibiting 24-Hour Periodicity
| Rhythm | Acrophase |
|---|---|
| Sleep | Night |
| REM Sleep | Night |
| Exercise capacity | Day |
| Activity | Day |
| Core temperature | Day |
| Hydroxicorticosteroid excretion in urine | Day |
| Adrenalin and noradrenalin production | Day |
| Cognitive performance | Day |
Source: USAARL, pg. 325
Internal and External Synchronization
Under a consistent environmental LD cycle, physiological and behavioral rhythms maintain a relative synchronization with each other (internal synchronization) and with the daily rhythm of sunrise and sunset (external synchronization). That is, in steady state conditions, they exhibit their peaks and troughs at approximately the same time of day or night, depending on their natural expression.
Source: USAARL, pg. 324
Your body does have a normal day/night cycle to it and this forms a rhythm where your normal active period is better suited to the day and your normal inactive period is better suited to night.
The body's natural clock and sleepiness
Since activity/rest rhythms exhibit an endogenous period greater than 24 hours (approximately 25 hours per day), it is easier to adjust to westbound travel, which results in a longer day.
Source: USAARL, pg. 326
When people live alone in environments from which all possible time cues have been carefully excluded (deep caves, underground bunkers, or specially designed apartments), they begin to live “days” that are generally longer than 24 hours. Regardless of how long someone’s subjective “day” becomes in a time-free environment, however, the circadian clock still enforces an approximately 25-hour cycle in many functions. Some people even develop “days” as long as 50 hours with, for example, 36 hours of wakefulness followed by 14 hours of sleep.
Source: NASA, pg. 22
We are physiologically programmed for two periods of maximal sleepiness in a usual 24-hour period. The period 3–5 A.M. is a circadian low point for temperature, performance, and alertness. During this time, the brain triggers sleep and sleepiness. The other period of increased sleepiness is roughly 3–5 P.M. Most individuals have experienced an afternoon wave of sleepiness. These windows can be used to schedule sleep periods or naps because the brain provides a period of maximal sleepiness and an increased opportunity for sleep.
Source: NASA, pg. 20
Maximal sleepiness occurs between 0600 and 0800. Although not as imposing, another episode of sleepiness occurs between 1400 and 1600.
Source: FASMB, pg. 1
Your natural rhythm is not based on a local clock but an internal one. For most of us it ends up being a 25 hour day, but that varies with individuals. Most of us, however, are forced to live in a 24-hour day. If you are programmed to a normal 2400 midnight and 1200 noon day/night schedule, then you will be sleepiest between 0300 - 0500 and 1500 - 1700 according to most studies.
2
Desynchronosis and jet lag
Individuals who engage in rapid transmeridian travel (e.g., airline crews) undergo alterations in the timing of the CTS. These changes manifest in the desynchronization of physiological and behavioral rhythms. Upon arrival, travelers encounter a new rhythm of sunrise and sunset and social schedule. The impact of these changes on body physiology results in several days of fatigue, sleepiness, lethargy, insomnia, gastrointestinal track disorders, and poorer mental agility and performance.
Source: USAARL, pg. 324
"Morning" versus "Night" People
Morning people ("larks"), with strong preferences for early morning wake up times, exhibit early morning peaks and large amplitudes in their temperature rhythms. These characteristics make the circadian system rigid and result in a greater resistance to resynchronization. In contrast, evening people ("owls") appear to have a more labile circadian system exhibiting smaller amplitudes in temperature rhythm than "larks," their peaks occur later in the day.
Source: USAARL, pg. 333
Age
A NASA study of the effects of aging found that as flight crews get older, they become more morning-type and the amplitude of their circadian temperature rhythm declines. Daily percentage sleep loss during trips was 3.5 times greater among long-haul crews aged 50–60 than among long-haul crews aged 20–30.
Source: NASA, pg. 29
Not everyone suffers equally from jet lag. Generally speaking, younger people and "night owls" do better crossing time zones.
The effects of jet lag on performance
In general, psychomotor performance after a 6-hour transmeridian flight suffers a reduction of 8-10% of preflight levels during the first day after arrival.
Source: USAARL, pg. 327
Sleep loss leads to increased waking sleepiness. Many people equate sleepiness with being lazy or acknowledge it only humorously. Sleepiness can have severe consequences for us as individuals and as a society. Sleepiness can degrade essentially every aspect of human performance. Sleep loss and sleepiness can decrease physical, psychomotor, and mental performance, and can increase negative mood and decrease positive mood. Therefore, a principal consequence of sleepiness is an increased vulnerability to performance decrements. It is important to consider this as a performance vulnerability because, like the effects of alcohol on performance and memory, sleepiness can lead to a reduced safety margin and an increased potential for operational incidents and accidents. Sleep loss and sleepiness resulting from extended duty or altered work/rest schedules have been suggested as contributory factors in many accidents and catastrophes. Many people put themselves at personal risk by driving when too sleepy, sometimes experiencing a near incident or an actual accident.
Source: NASA, pg. 28
- Reaction times may be markedly slowed, which can be critical when rapid reactions are necessary.
- False responding also increases, i.e. the pilot may take action when no action is warranted, especially when aware of having missed signals. The resulting anticipation of another event and over attention on individual signals or problems further reduces situational awareness.
- Fatigue increases calculation errors, logical errors, and ineffective problem solving. The member is less able to think of new solutions and repeatedly tries the same approach to a situational problem.
- Memory deficits progressively worsen with fatigue and sleep loss.
- The sleepy and tired crewmember reads or hears instructions repeatedly but cannot retain the information, leading to critical errors and uncertainty about the status of the situation.
- Performance variability results from increased lapses and errors of omission.
- Although the member often becomes aware of the shortcomings in performance and responds by trying to increase self-motivation and effort, performance improvement is short-lived. He/she may perceive the operation as more stressful and tiring as the effort continues. Ultimately, the crewmember's motivation to perform well and avoid risks erodes.
Source: FASMB, pg 2
It is said that the effects of fatigue are similar to alcohol. You don't react as quickly or accurately, you don't remember things as well, and your motivation to do things correctly suffers as well. On top of all that, you become less critical of yourself and therefore become a poor judge of your own performance.
3
Subjective vs. physiological sleep and alertness
- It is usually difficult for most individuals to reliably estimate their own sleep or their waking alertness, especially if they are already sleepy.
- Overall, there is a tendency for individuals to subjectively overestimate how long it takes to fall asleep and underestimate total sleep time, relative to physiological measures. Generally, people fall asleep faster and sleep longer than they think. So when an individual experiences a bad night of sleep, it may not be as bad as it seemed.
- However, the tendency is for individuals to subjectively rate themselves as more alert than is indicated by physiological measures. That is, most individuals are more likely to be sleepier than they report or experience.
Source: NASA, pg. 18
Odds are that you are falling asleep faster than you think and sleeping longer than you give yourself credit. But you are also probably more sleepy thank you think too.
4
Coping strategies
Preventive strategies (before the trip)
- Prior sleep loss can be a significant factor in the severity of subsequent jet lag symptoms. That is, individuals who are sleep deprived before a trip can experience more difficulty than those who are well rested. An individual who begins a trip with a sleep debt, should expect that the it will only worsen during the trip schedule. The recommendation is to begin a trip schedule as sleep-satiated as possible. Maximize the amount of sleep at least 1 and preferably 2 days before departure.
- Most flight operations are characterized by sleep loss during trip schedules. Individuals should attempt to obtain at least as much sleep during a layover as they would typically during a normal 24 hours at home. Knowing that circadian and other factors will diminish the physiologically available windows for sleep, attempts should be made to maximize these opportunities.
- Learn to trust your own physiology. When struggling to stay awake, take the sleepiness as a clear sign to get some sleep. Instead of fighting the sleepiness, take a brief nap or a longer sleep time. Also, if after awakening spontaneously you are unable to return to sleep within 15–30 minutes, then get out of bed. The principal message is that if your brain is giving you clear signals that you are sleepy, then sleep. If you awaken and you are alert and unable to return to sleep, get up. You can force wakefulness, but you cannot force sleep.
Source: NASA, pg. 45
- First, keep a regular sleep and wake schedule as much as possible. At home before trips, try to keep sleep time protected and minimize other responsibilities. A regularly practiced pre-sleep routine can be used to teach your mind and body that it is time to relax and fall asleep. A set of cues can be established to condition pre-sleep relaxation and can then be used anywhere and anytime before going to sleep. It is important to avoid work or worry in the bedroom and to prevent the association of the bed with activities contrary to relaxation and sleep.
- Going to bed hungry can delay falling asleep. Eating a heavy meal also can disrupt sleep, for the stomach is busy digesting food. If hungry or thirsty at bedtime, eat a light snack or have a small quantity of something to drink. Alcohol should be avoided immediately before going to bed because of disruptive effects on sleep. Caffeine consumption should also be limited. Caffeine in coffee, tea, and colas can prevent sleep onset and disrupt subsequent sleep. Some individuals are sensitive to the caffeine in chocolate, and even a chocolate dessert after dinner is enough to interfere with their sleep. Many mild pain relievers also contain caffeine; read the label for ingredient information. Be sure to stop caffeine intake several hours before planned bedtime.
- If unable to fall asleep in 30 minutes, don’t lie in bed trying to fall asleep. Instead, get out of bed and engage in some activity conducive to relaxation and sleep.
- Disruptive environmental factors should be minimized. Sleep in a dark, quiet, temperature-controlled room, and on a comfortable sleep surface.
- Laboratory studies suggest that regular exercisers may have increased amounts of NREM stages 3 and 4. However, exercising too close to bedtime can disrupt subsequent sleep. Although physically tiring, exercise elevates heart and breathing rates, and is generally activating physiologically. Usually, it is not possible to immediately wind down and fall asleep after exercise. A balanced diet and regular exercise are critical components for overall good health.
Source: NASA, pp. 47-48
- Use the bed primarily for sleep.
- Avoid looking at the time. Set an alarm and ignore the time.
- Avoid alcohol, caffeine, and heavy meals before bed.
- Schedule a worry time, planning session, and wind-down time before getting into bed. Make lists of things to do the next day.
- Make the bedroom quiet, comfortable, dark, and secure. Use white-noise generators if the environment is noisy. Minimize disruptions.
- Get out of bed after lying awake for more than 20 minutes-do something boring or try relaxation techniques.
- Avoid exercise and hot baths within 3 hours of bedtime.
- Exercise regularly, in the morning or afternoon.
- Keep a regular bedtime and get-up time.
- Do not spend excessive amounts of time in bed, e.g., if you can sleep only 7 hours, spend no more than 7.5 hours in bed.
- Avoid excessive napping, which can interfere with your ability to sleep at night.
Source: FASMB, pg. 5
Make a ritual about sleeping at home. Get rid of the bedroom television to train your brain that the bed is for sleep. Get into a regular schedule so that prior to bedtime you do the same things, avoid heavy exercise, eating, drinking, and go to bed. Get up at regular times too. If you can't fall sleep in 30 minutes, don't lie in bed awake. Get out of bed for a while and do something relaxing.
Strategic napping
- An extensive scientific literature clearly demonstrates the effectiveness of naps in improving subsequent alertness and performance. One important consideration when napping close to a duty period is to minimize the chances of going into deep NREM sleep (stages 3 and 4). If awakened out of deep sleep, an individual may continue to feel groggy, sleepy, or disoriented for 10–15 minutes. This phenomenon is called sleep inertia. Therefore, if taking a nap before a duty period, limiting its duration to 45 minutes or less will decrease the chances of having significant amounts of deep sleep. A brief nap can be an important way to decrease the length of continuous wakefulness. It is usually much better to get some sleep than none at all.
- When you nap at times other than immediately before a duty period, then the nap can be longer. In this case, a nap longer than 2 hours is likely to get an individual through at least one NREM/REM cycle.
- Strategic napping can be an extremely effective countermeasure in improving subsequent alertness and performance. Some individuals call these “power” naps. In flight operations, “NASA naps” have been demonstrated to be an effective acute fatigue countermeasure.
Source: NASA, pg. 46
If you can take a nap, time it appropriately. If you have to be on duty within an hour or so, limit the nap to 45 minutes to prevent deep sleep. If you have enough time to fully awaken following the nap, then a nap longer than 2 hours is permitted.
Operational strategies
- Operational countermeasures are challenged by FARs that require crewmembers to remain seated at their assigned duty stations with their seat belts fastened. This poses a challenge because one of the most successful technique for combating sleepiness, according to the earliest sleep-deprivation experiments, is physical activity. Whenever possible, engage in physical activity, even if it is only stretching. Take regular stretch breaks and while seated remain as active as possible—even writing helps. Engage in conversations with others and be sure to participate; don’t just nod and listen.
- Caffeine, a stimulant, can be consumed strategically to acutely increase alertness. It is best not to continually consume caffeine before, during, and after a trip. Instead, determine the potential periods when caffeine could be used to combat a specific period of sleepiness (e.g., 3–5 A.M. or 3–5 P.M.). Avoid using it when already alert, for example, when just beginning a daytime duty period or immediately after a nap. Though affected by several variables (e.g., body size, previous food intake), caffeine will usually take 15–30 minutes to take effect and then last for up to 3–4 hours. Therefore, continually consuming caffeine throughout a flight could interfere with subsequent sleep on layover. Stop caffeine consumption far enough in advance of a planned bedtime so that it will no longer be active.
- Be sensible about nutrition. Whenever possible, maintain a balanced diet. Obviously, flight operations can interfere with regularly scheduled, balanced meals. Try to carry appropriate snacks as needed. Drink plenty of fluids and stay hydrated. Between reduced cockpit humidity and caffeine (a diuretic), it is easy to become dehydrated.
Source: NASA, pg. 49
5
Resynchronization
Adjusting to the New Time Zone
Transmeridian travelers who expect to remain in the new time zone for weeks should quickly change the timing of behavior patterns to match local events, that is, sleep and wake-up times, meal times, and social events should match local schedules as soon as possible. To speed up the rate of readjustment, it is necessary to (1) immerse oneself in local society, maintaining normal social activity patterns, (2) engage in physical exercise, and (3) maintain regular exposure to daylight.
Source: USAARL, pg. 328
Remaining on Home Base Time
In certain circumstances, travelers can attempt to maintain the time schedule of their departure location by not resetting their watches and by scheduling events, meals, and sleep times to match their home base clocks. This technique avoids most of the CTS disruption of travel except for the change in LD cycle.
Source: USAARL, pg. 328
Sleep Timing
Because getting uninterrupted restful sleep upon arrival is often difficult, the traveler should be fully rested at departure so there is no "sleep debt." A wristwatch can be set to the destination time zone and activities pursued according to the next clock time. Bedtime should be shifted progressively earlier each night (phase advance) for a few days before an eastward flight and progressively later (phase delay) in anticipation of a westward flight. The time of awakening must also be adjusted.
Source: USAARL, pg. 328
The problem with having to get up earlier than usual is that it is very difficult, if not impossible, to fall asleep sufficiently early the night before to compensate (even when the duty schedule permits). It is not simply a question of discipline or motivation. The circadian clock effectively opposes falling asleep earlier than the habitual bedtime. Just as there are preferred times in the circadian cycle for falling asleep, there are also times when sleep onset is very unlikely. These times have been labeled “wake maintenance zones,” and one of them occurs just before the habitual bedtime. In addition, because the “biological day” dictated by the circadian clock tends to be longer than 24 hours, it is easier to go to sleep later than to go to sleep earlier. Going to sleep later also means staying awake longer, which allows more time for the homeostatic “sleep pressure” to build up.
Source: NASA, pg. 36
Meal Timing and the Use of Diets
Diet has not, however, been shown to aid in actual resynchronization of the CTS. . . . Although choice of meals may possibly aid in inducing sleep or alertness, it is the consistent timing of meals and fasting periods that will serve as phase information for the oscillator influencing the GI track and that will ultimately play a significant role in facilitating CTS resynchronization.
Source: USAARL, pg. 329
Alcohol
Alcohol has a profound effect on the usual sleep cycle. After more than a couple of glasses of wine or a couple of beers (with individual variations), alcohol can essentially eliminate all of the REM sleep in the first half of a sleep period. This can lead to subsequent alcohol withdrawal effects in the second half of the sleep period, including sleep fragmentation. Unfortunately, the most widely used sleep aid in the United States is alcohol. Ironically, although often used to promote relaxation and the ability to fall asleep, it will generally have major disruptive effects on the subsequent sleep. One NASA study found that short-haul pilots increased their alcohol consumption threefold during trips compared with home consumption. The pilots used alcohol within FAR guidelines to unwind after long duty days that included multiple flight segments and to promote sleep onset before an early wake-up for the subsequent duty day. Alcohol also interacts in a synergistic fashion with sleepiness. A sleep-deprived individual who is already sleepy will demonstrate more severe performance and alertness impairment following alcohol consumption.
Source: NASA, pg. 14
Bright Light Therapy and Jet Lag
Bright artificial lights may be used to mimic the destination LD cycle before the transmeridian flight. In this manner, travelers may reduce to desynchronosis experienced upon arrival.
Source: USAARL, pg. 329
Bright light has been shown in laboratory studies to facilitate rapid circadian adaptation. Two to three hours of bright light (i.e., 2,500–10,000 lux) administered at the appropriate phase of the temperature cycle for three successive days may facilitate an 8- to 12-hour shift of the circadian clock. Separate from its effects on the circadian clock, bright light also can have an independent alerting effect.
Source: NASA, pg. 52
Resynchronization
In general, the human CTS exhibits a preference for quicker reestablishment of internal synchronization after a delay in the activity/rest rhythm or LD cycle.
Source: USAARL, pg. 332
Another commonly held belief is that after sleep loss, an individual has to “make up” that sleep by sleeping a number of hours equal to those lost. Scientific laboratory studies have demonstrated that following sleep deprivation, recovery sleep is deeper (more NREM stages 3 and 4), rather than extended. During recovery sleep, an individual might sleep somewhat longer, but the most notable feature is the increase in deep sleep.
Source: NASA, pg. 13
As corporate pilots we rarely have the opportunity to fully "sync up" with our new environment before it is time to go home or move further away from our normal biological clock. It has been my experience the following strategy works best for me:
- Before leaving home, try to sync up with the destination time zone a few hours, if possible. If going east, try to shift your night activities later in the day; if going west, shift earlier.
- During flight, get out of the seat whenever feeling drowsy, if possible. Engage the rest of the crew in conversation. Make a ritual of performing certain tasks to an extra level of detail. Plotting charts, for example, offer lots a room for creativity.
- Plan your caffeine for about 20 minutes prior to when you need it the most.
- When adjusting to a new time zone, sleep when you are tired. If you will be in the new time zone for a few days, try to limit your local day naps to a few hours at most.
- If you are planning another long flight day, work to bring the next flight's duty time into your normal "day" activity.
- For example, if you leave Boston for London late at night with a 8 a.m. local arrival, you may be tempted to go to bed immediately. But if your next flight is in a day, further east to Israel, you might want to rethink that. Say your next flight will be departing London early in the morning. It will be in your best interest to attempt to realign your circadian rhythm as best you can so as to be better rested for the next long flight. I would limit my nap in London to a few hours and attempt a more normal sleep that night.
- If, on the other hand, you have a Boston - Paris trip with a Tuesday 5 a.m. arrival followed by a return on Wednesday departing at noon, your best bet may be to forgo the Eifel Tower and keep on East Coast U.S. time. (You arrived at 11 p.m. Boston time, ready for bed. Go to bed and sleep for eight hours. Get up around 1 p.m. Paris time and don't plan on going back to bed until later that night. The next day you are leaving at 6 a.m. Boston time, ready for the day.)
References
(Source material)
Harris, Sydney, "You Want Proof? I'll Give You Proof!" More Cartoons from Sydney Harris, 1990
NASA 2002: Crew Factors in Flight Operations XV: Alertness Management in General Aviation Education Module, NASA, February, 2002.
FASMB 2006: Fatigue and Desynchronosis in Air Crews, Federal Air Surgeon's Medical Bulletin, Summer 2002.
USAARL 1990: Circadian Rhythm Desynchronosis, Jet Lag, Shift Lag, and Coping Strategies, Carlos A. Comperatore and Gerald P. Krueger, United States Army Aeromedical Research Laboratory, Biomedical Applications Research Division, September 1990.